By Neena Bhandari
Sydney, 22.07.2021 (The Medical Republic): Major cancer hospitals across the country are offering oncology massage as one of the tools in their integrative oncology and support centres to help some people cope better with treatment.
When Marcia Sherring underwent a bilateral mastectomy and related surgeries followed by chemotherapy and radiotherapy, her surgeon referred her to the integrative oncology service at the Chris O’Brien Lifehouse, a comprehensive cancer hospital in Sydney. She was recommended oncology massage for her lymphedema.
At first, she was hesitant. “I looked like an extra from a war movie with lots of scars and stitches on my body. But to my surprise, the oncology massage therapist wasn’t shocked. She seemed to have complete knowledge and understanding of my medical history and she modified her technique to account for the adhesions and scarring on my chest. It made me feel safe and confident in her hands”, says Sherring.
Sherring is among a growing number of people living with cancer, who are benefiting from using Integrative Medicine, which combines the best of conventional western medicine with evidence-based complementary medicine and therapies, such as oncology massage.
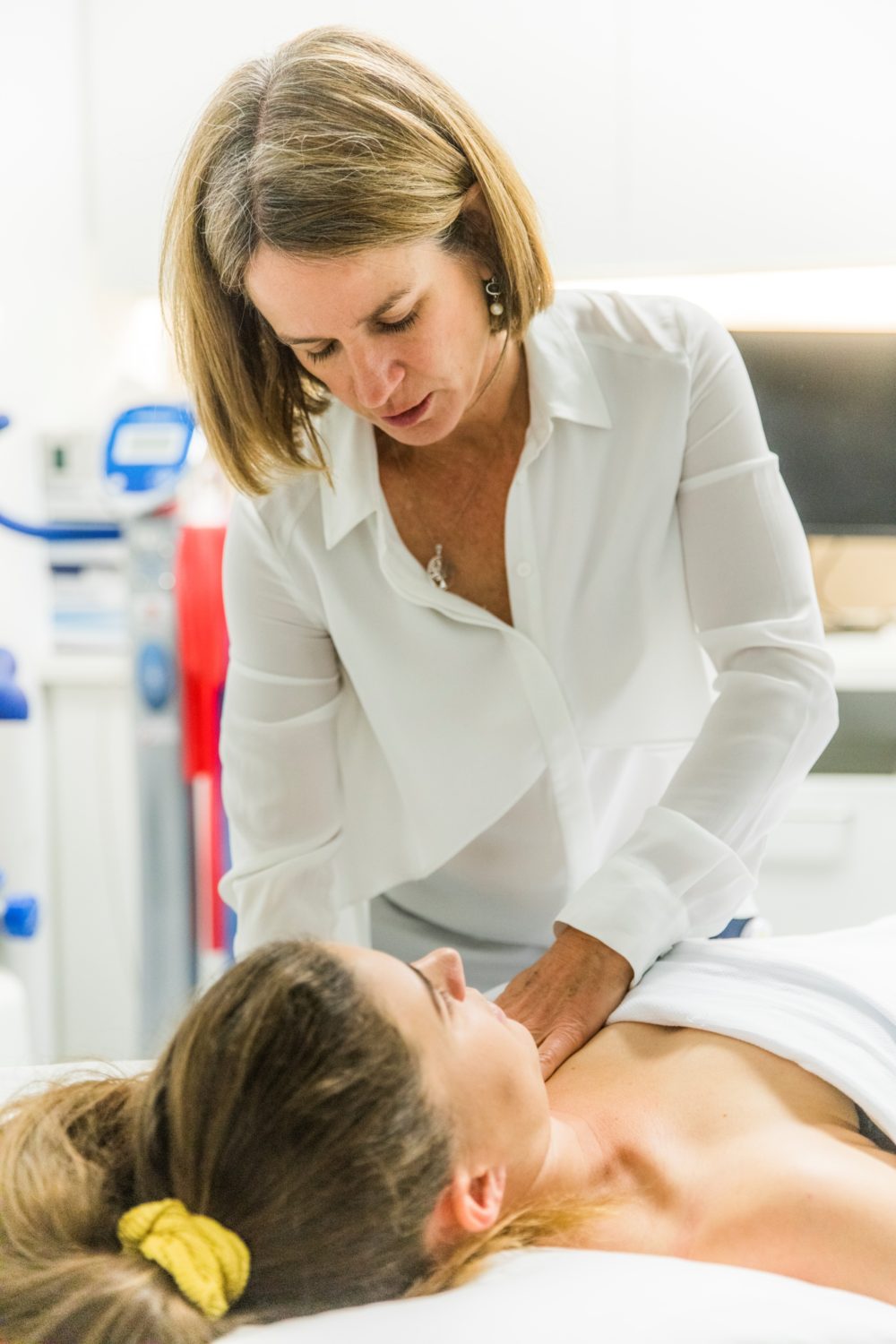
“What differentiates oncology massage from regular massage is its goal. Regular massage is focused on fixing the body, for example musculoskeletal problems or sporting injuries. Oncology massage is about nurturing the body by using gentle fascial mobilisation to create a “Relaxation Response” demonstrated by founder of Harvard’s Mind Body Medical Institute, Dr Herbert Benson”, explains Eleanor Oyston, who established Oncology Massage Training in Australia in 2003 after working for three decades in developmental neuroscience and cytology, diagnosing cancer.
Oncology massage therapists are imparted specialised knowledge about cancer, its treatment and impact, especially haematological cancers. “They are trained to adapt their technique — position, pressure, duration and area treated — to each patient’s specific needs”, says Oyston, who is currently CEO of Oncology Massage Global. “This allows them to deal safely and effectively with situations such as lymphoedema, neutropenia, lowered blood counts, bone metastases, wound sites, clotting abnormalities, skin sensitivity; and surgical devices such as catheters, ports and stoma bags.”
According to Dr Carol Haddad, a Radiation Oncologist who combines conventional and complementary medicine in her Integrative Cancer Care practice in Sydney, safety is the most important factor to consider with oncology massage.
“Lymphatic drainage massage is the most common type of oncology massage used in the conventional medical setting. For example, following dissection of the lymph nodes in breast and pelvic cancer patients, lymphatic fluid can be massaged away from the areas of accumulation”, says Dr Haddad. “It is now gaining popularity for relieving pain, reducing scar tissue formation following surgery and improving the symptoms and side effects of cancer and its treatment.”
“But the massage therapist needs to take into consideration any active sites of disease and active symptoms, any change in anatomy from surgery, and it should not interfere with wound healing”, she cautions. “I would be careful not to recommend massage in the areas being treated during active radiotherapy and during some chemotherapy regimens which can cause hypersensitisation to touch”.
Clinical studies have shown that massage can help ease stress, anxiety, pain, nausea, insomnia, fatigue and depression in cancer patients. According to a 2004 research on the benefits of massage from the Memorial Sloan-Kettering Cancer Center in New York, there was 47 percent reduction in pain, 51 percent drop in nausea, 42 percent improvement in fatigue levels, 59 percent improvement in anxiety levels and 48 percent improvement in depression.
Associate Professor Haryana Dhillon, Senior Research Fellow in Psycho-Oncology at the University of Sydney says, “We often find people with psychological distress associated with their cancer will not be open to seeing a psychologist or a counsellor. Sometimes, a massage and interaction with their massage therapist, can help to introduce the idea of psychological support. So oncology massage does have a role to play for some cancer survivors”.
The Society for Integrative Oncology (SIC) has credentialing guidelines for oncology massage therapists. The Cancer Council of Australia has a booklet on massage. Several cancer hospitals offer it, including Chris O’Brien Lifehouse and the Kinghorn Cancer Centre in Sydney; and Olivia Newton John Cancer and Wellness Centre and Peter MacCallum Cancer Centre in Melbourne.
Dr Judith Lacey, Head of Integrative Oncology and Supportive Care at Chris O’Brien Lifehouse, sees oncology massage as an integral component of holistic supportive care from the time of cancer diagnosis through to survivorship and end of life care. She says, “People with cancer need to be treated with an expanded toolbox and not just for the symptoms of the disease. The benefit of non-pharmacological treatments, which also reduce polypharmacy, are gaining interest”.
Research has shown oncology massage may help restore homeostasis, reduce cortisol and inflammatory markers, increase dopamine, improve chemotherapy-induced peripheral neuropathy and release muscle spasm.
“The challenge is understanding the mechanism that makes people heal and feel better and showing the benefit for specific symptoms, which is difficult to evaluate in a Randomized Controlled Trial, but it is possible as an implementation science. We are still exploring what happens as a result of massage when working in the fascia level on neurotransmitters, inflammatory mediators such as cytokines and perhaps even endocannabinoids”, says Dr Lacey, who is also Chair of the Clinical Oncology Society of Australia and Co-Chair of SIC’s Clinical Practice Group.
In 2016, researchers at Western Sydney University’s (WSU) NICM Health Research Institute surveyed public and private healthcare organisations that provide specialised cancer services in the country and sought cancer survivors’ views and their experiences with different types of complementary medicine. This national study found the main barriers to providing oncology massage were funding and finding qualified oncology massage therapists.
“There is gross underfunding of allied health and complementary medicine services for cancer recovery and rehabilitation. Healthcare spending focuses on treating and curing, which is dominated by chemotherapy, radiotherapy and surgery, and the infrastructure needed to deliver these services”, says Dr Jennifer Hunter, Adjunct Associate Professor at WSU and co-investigator of the study.
The idea of integrating massage into cancer treatment is slowly becoming more accepted in the United States, the United Kingdom and some European countries.
Dr Hunter says, “In our 2016 study, we found that only 66 hospitals out of the 262 surveyed offered complementary medicine cancer services and a secondary analysis confirmed that massage is yet to be firmly established in cancer care in Australia. It is often seen as an adjunct luxury item, yet some patients held a very different view about its value”.
To make oncology massage more acceptable and encourage the medical profession to integrate it in cancer care, Dr Haddad says, “We need more research studies demonstrating clear benefits of using massage; educate and train massage therapists in using safe techniques and in the contraindications to massage; improve access to oncology massage by creating smooth pathways for referrals; and make it more affordable either through bulk billing under Medicare or subsidised by private health funds”.
Oncology Massage gaining acceptance in cancer care
Continue Reading on The Medical Republic
© Copyright Neena Bhandari. All rights reserved. Republication, copying or using information from neenabhandari.com content is expressly prohibited without the permission of the writer and the media outlet syndicating or publishing the article.